- Have Questions
And Need Answers?
LIVE CHAT NOW! - COMPLIMENTARY CASE EVALUATION
Need Help? Call Us Today!
877-773-3030
Schedule A ConsultationExperience You Can Trust
Yes, VA disability benefits for ischemic heart disease may be available.
You will need to prove that (a) you were in the military, (b) your ischemic heart disease originated or was aggravated while you were on active duty, (c) you were continuously treated for your ischemic heart disease since leaving the service (unless you are filing your disability claim within one year of leaving the service or your condition has been chronic), and (d) you are currently disabled by your ischemic heart disease.
Ischemic heart disease (IHD) is a major medical problem disabling and killing millions of people in the U.S. yearly, and therefore a frequent basis for allegations of disability.
Heredity plays an important role, but so does lifestyle. Many IHD deaths are preventable and associated with poor control of hypertension and diabetes mellitus, smoking, lack of exercise, obesity, and poor diet resulting in elevated blood lipids (fats such as cholesterol).
Ischemia means that the heart (or other body tissue) is not receiving enough oxygen to function normally. The oxygen demands of the heart change with heart rate. So increased heart rates require increased blood flow to the heart to deliver the oxygen and glucose needed for the extra work. Ischemia not present at rest may appear when the heart rate increases, and this is the basis for cardiac stress testing.
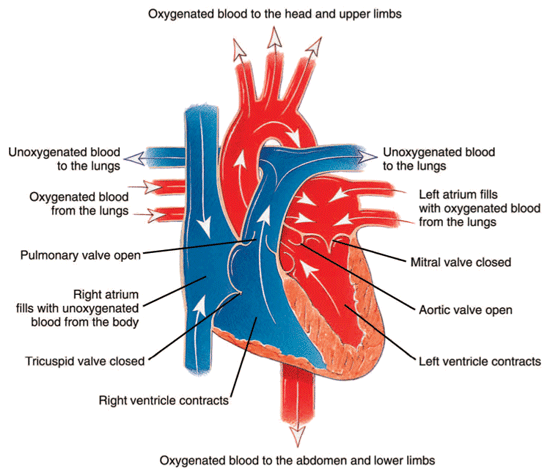
Figure 1: The path of oxygenated and unoxygenated blood in the heart during contraction.
Most IHD results from obstruction of the coronary arteries that supply the heart muscle with blood. This condition is known as coronary artery disease (CAD). Other cardiac abnormalities can also cause myocardial ischemia. The underlying mechanism is still the same: restriction of blood flow to the heart muscle (myocardium). For example, marked narrowing of the aortic valve can cause chest pain because the coronary arteries originate right above the valve and may not receive sufficient blood flow to supply the heart. However, the great majority of claimants have myocardial ischemia because of CAD.
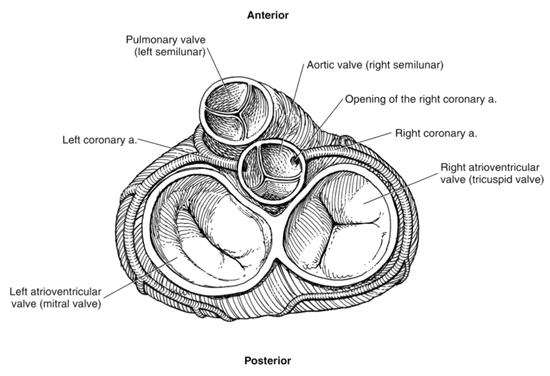
Figure 2: Closed heart valves.
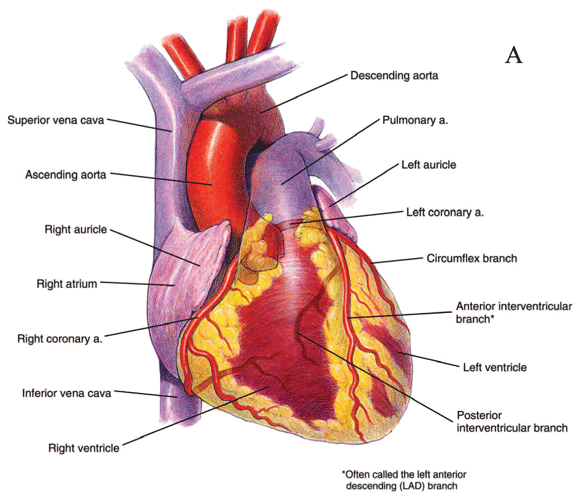
Figure 3: Anterior view of the heart, including main arteries.
Blood flow to the myocardium served by a particular coronary artery is not significantly decreased until a lesion blocks about 70% of the diameter of the artery. It is frequently possible for a person to be comfortable at rest with a 90% blockage in a large epicardial artery.
Lesions of less than 50% are generally considered to not be significant CAD, because the heart will still be able to obtain sufficient blood flow both at rest and with exercise. However, this conclusion must be made in context of all of the medical evidence. Long segments of obstruction rather than discrete lesions, involvement of the left main coronary artery, or involvement of multiple arteries could cause significant ischemia with blockages as low as 50%.
Ischemia can be indicated by:
Cardiac stress testing raises heart rate to determine:
1) Whether ischemia can be induced,
2) The level of exertion producing ischemia, and
3) The severity and location of the ischemia.
In exercise stress testing, your baseline ECG is obtained. Then you begin with a low level of exercise, either by walking on a treadmill, or pedaling a stationary bicycle. Every two to three minutes, the level of exertion is increased. At each stage of exercise, your pulse, blood pressure and ECG are monitored are recorded, along with any symptoms you may be experiencing.
The exertion level is gradually increased until you cannot keep up any longer, or until your symptoms (chest pain, shortness of breath, or lightheadedness) prevent further exercise, or until changes on your ECG indicate a cardiac problem.
There are other means of raising heart rate for testing purposes, such as pharmacologic stress testing in which drugs are used to raise the heart rate. Pharmacologic stress testing can be used with patients who, for some reason, cannot perform exercise stress testing.
Both exercise testing and pharmacologic testing can be used in conjunction with various types of imaging studies of the heart’s response to increased heart rate—such as radionuclide scans or echocardiograms that are done at the same time.
Common symptoms of myocardial ischemia are: