- Have Questions
And Need Answers?
LIVE CHAT NOW! - COMPLIMENTARY CASE EVALUATION
Need Help? Call Us Today!
877-773-3030
Schedule A ConsultationExperience You Can Trust
Yes, VA disability benefits for stroke may be available.
You will need to prove that (a) you were in the military, (b) your stroke originated or was aggravated while you were on active duty, (c) you were continuously treated for your stroke since leaving the service (unless you are filing your disability claim within one year of leaving the service or your condition has been chronic), and (d) you are currently disabled by your stroke or other anxiety disorder.
A stroke is called a cerebrovascular accident or CVA by medical professionals. It is usually caused by either:
Most strokes are caused by cerebral infarction in which an artery in the brain is blocked depriving the brain of blood and damaging brain tissue.
An arterial thrombosis (blood clot) is the most common cause of cerebral infarction. Such a clot could form in a cerebral artery itself or in the heart as a result of a variety of heart problems and be pumped to the brain. Blockage of a cerebral artery by the fatty deposits of atherosclerosis can also deprive an area of the brain of blood and lead to infarction. Actually, many cerebral infarctions are caused by cerebrovascular disease in which a blood clot forms around fatty plaques.
Unlike arteries in the heart or legs, cerebral arteries cannot be cleaned out of fatty blockages. However, if a stroke occurs as a result of a blood clot, brain damage can be lessened by clot-dissolving drugs. Medical attention must be sought within a few hours for treatment to be effective and clot-dissolving drugs pose some risk of causing deadly bleeding.
A piece of atherosclerotic plaque can break off inside one of the two internal carotid arteries in the neck, be pumped to the brain, and lodge in a cerebral artery to cause an infarction.
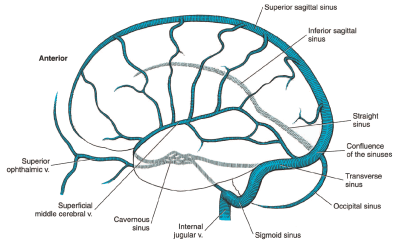
Figure 1: Veins of the brain.
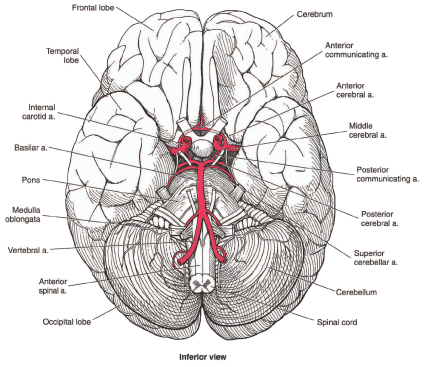
Figure 2: Base of the brain, including main arteries.
The most frequent cause of hemorrhagic CVAs is uncontrolled hypertension (high blood pressure), often related to non-compliance with medical treatment. Bleeding in the brain may also occur from abnormal tangles of blood vessel growths called vascular malformations and cerebral aneurysms.
A significant number of strokes are caused by cerebral aneurysms, which are enlarged and weak areas of a cerebral artery that can rupture and cause a subarachnoid hemorrhage (SAH). Aneurysms in the cerebral circulation are common. They are estimated to occur in between 1% and 5% of the general population and account for 5% to 15% of strokes.
The most common location for cerebral aneurysms is the anterior cerebral artery. Cerebral aneurysms are twice as common in women as in men. They occur more frequently in individuals with certain disorders such as autosomal dominant polycystic kidney disease. More than one aneurysm may be present.
Millions of Americans have cerebral aneurysms. Although somewhere between 50% to 80% of aneurysms are small and do not rupture—many are only found incidentally at autopsy—that still leaves millions of individuals at risk for death or debilitating stroke.
If a stroke occurs, the prognosis is grave, with a mortality of about 40% to 50% within 30 days of the first rupture. For surviving patients with SAH, about 30% have significant neurological abnormalities. For instance, following SAH, 15% to 20% of individuals will develop hydrocephalus (fluid accumulation on the brain) and require further neurosurgical procedures to treat that serious brain disorder.
If a person has experienced one rupture (bleeding episode) from an aneurysm, the risk of future bleeding is increased to 10 times that of someone with a no rupture history. If the aneurysm was large (10 mm or more), the risk of rebleeding is even higher.
If an aneurysm has not bled previously, data indicates a low bleeding risk of 0.05% per year; in aneurysms less than 7 mm, the 5-year risk approaches zero in the absence of a bleeding history. However, the size of an aneurysm is not the only consideration—aneurysms putting pressure on vital brain structures, such as a cranial nerve, require surgical intervention at a smaller size.
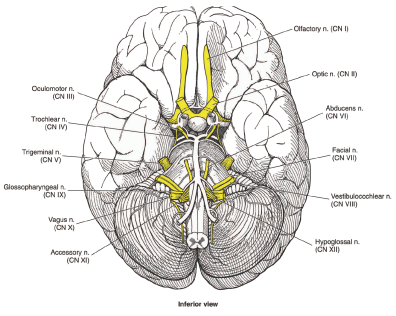
Figure 3: Cranial nerves at the base of the brain.
Evidence that a cerebrovascular accident or CVA has occurred is based on history and physical examination, as well as neuroimaging with computerized tomographic angiography (CTA) or magnetic resonance angiography (MRA) of the brain.
Cerebral catheter angiography, a much older procedure than CTA or MRA, is still sometimes used. It carries some risk and is not needed to evaluate most CVAs. Cerebral catheter angiography involves direct injection of x-ray contrast material to outline the arteries of the brain. A catheter is threaded through the femoral artery in the leg, up into a carotid artery in the neck, and then manipulated into the cerebral circulation where contrast injection takes place.
Brain cells that are killed by a stroke are not replaced with new cells. The brain cannot re-grow any part of itself. But it can re-arrange brain cell connections to some degree to compensate for injury. The ability of the brain to compensate for injury decreases with age. Recovery from stroke depends on the ability of remaining brain areas to perform necessary functions, and recovery of areas not permanently damaged by the CVA.
Rehabilitation is very important in achieving maximum possible recovery, and should be instituted as soon as possible after the CVA.
CVAs can be of all degrees of severity, and the type of damage they do depends on where in the brain they occur. Some CVAs cause death immediately, while others may cause little limitation. There might be good recovery, or very little.
Strokes can have many effects depending on what areas of the brain are damaged:
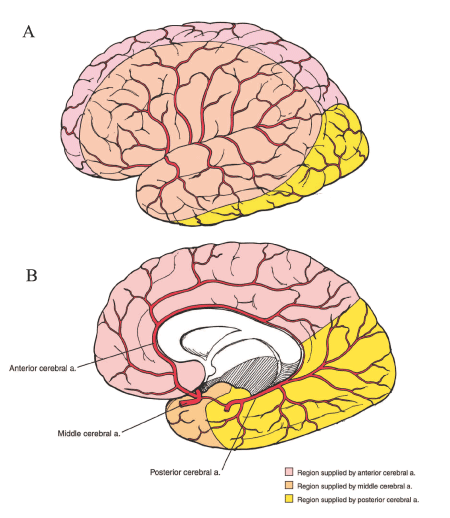
Figure 4: The Circle of Willis, showing main cerebral arteries and the parts of the brain they supply.
At a physical examination, a doctor can obtain information regarding strength in the upper and lower extremities with some simple and routine maneuvers. First, the examining physician can estimate strength loss by comparing the strength of muscle contraction on your weak side to your normal side.
Physicians frequently report subjective determination of strength by using a scale of 0 to 5 with 5 being normal. For example a doctor might ask you to try to straighten out your leg while the doctor resists the movement. A weaker leg might be reported as 3/5 for the quadriceps muscle (muscle on the front of the thigh) compared to an expected normal of 5/5. Zero means no movement. One means a trace of movement. Two means movement with the help of gravity. Three means movement is possible against gravity, but not against resistance. Four means movement against gravity and resistance by the examining physician. Five means normal. Errors in this type of subjective testing can be caused by the person’s motivation, variations among people in “normal” strength, and differences in the doctor’s subjective assessment.
More objectively, a doctor can test your ability to walk on your heels and toes and squat and arise. Ability to walk on the toes means you can lift your body weight by contraction of your gastrocnemius (calf) muscles and implies significant strength. Ability to walk on the heels indicates that the muscles in the anterior (front) leg (opposite the calf muscles) that flex the foot still have good strength. Ability to squat and arise implies good strength of the quadriceps muscles of the thighs.
Determination of lower extremity strength after a stroke is very important. If you cannot walk on heels or toes in the affected lower extremity after a CVA, it is not reasonable to expect that you would have the strength to stand 6 to 8 hours daily.
Evaluating how well you stand and walk involves factors such as how weak your legs are, how much difficulty you have in keeping your balance, how fast you walk, how much help you need walking, and so forth.
After a severe CVA, walking (gait) and standing (station) may be affected in characteristic ways. If a leg and arm are weak from a CVA, a person will often walk with a circumducting gait. The weak leg moves forward with a circular motion and the weak arms has a short swing. On the other hand, a CVA in the brainstem or cerebellum may produce an unsteady (ataxic) gait, frequently with legs wide-based in an effort to compensate for the loss of balance.
Your balance can be tested in neurological examination not only by observing your normal attempts at walking, but also by testing your ability to walk heel to toe. If there is weakness of the pelvic musculature, a waddling gait may result. A foot drop tends to cause a steppage gait, lifting the foot high to clear the toes from the ground. Spasticity, produced by increased muscle tone, can produce a stiff limb with inflexible movements.
The use of the arms and hands is evaluated by looking at gross and dexterous movements. Dexterous movements are those like writing, picking up small objects, or other types of fine movements. Gross movements involve larger motions with the arms and hands. Movements can be influenced by weakness, or loss of control over the way an arm or hand moves, such as tremors or poor coordination.
The ability to oppose fingertips to the thumb successively can give some idea as to the intactness of fine manipulatory (dexterous) ability. However, if you can do finger-thumb opposition only slowly and clumsily, then you should not be considered capable of dexterous movements. Also, your activities of daily living (ADLs) can be helpful in assessing functional severity when they describe specific inabilities or abilities (e.g., turning doorknobs, dressing, climbing stairs, shaving, etc.).
Your medical history is very important. Claimants who have actually had a severe CVA have been hospitalized. The records from that hospitalization will provide a picture of clinical severity. The initial physical examination can be reviewed, along with the degree of recovery at the time of hospital discharge.
Almost certainly, a CT or MRI scan was done of the brain and sometimes cerebral angiography. These studies can be most helpful in determining the location and severity of brain damage, so that it can be correlated with the clinical findings at the time of adjudication. Some claimants allege abnormalities that were not present at the time of their CVA and do not correspond to the location or magnitude of the initial brain lesion, or they seem to manifest weakness much greater than that present in their past medical records.
If the claimant underwent rehabilitation in the past, that information is useful.
Certain objective signs are present after a CVA. Deep tendon reflexes (DTRs) in the affected parts of limbs should be hyperactive, or faster than normal. For example, tapping the patellar tendon below the knee (knee-jerk reflex) would cause the quadriceps muscle to more rapidly contract and the leg to extend more quickly than normal.
Reflexes are graded from 0 to 4. Zero (0) means no reflex. One (1) means a distinctly hypoactive (slow) and abnormal reflex. Two (2) andthree (3) mean a normal reflex. Four (4) means a distinctively hyperactive and abnormal reflex. Physicians usually report reflexes in a right/left mode. For example, a knee-jerk (KJ) reflex reported as 4+/2 indicates a very pathological KJ on the right. Reports of 2/2 or 3/3 for reflexes should be interpreted as normal. However, asymmetry in reflexes may be significant, e.g., 2/3+ might indicate an abnormal reflex on the left.
Additional basic reflexes important in neurological examination include the achilles reflex (AJ), biceps jerk (BJ), triceps jerk (TJ), and brachioradialis reflex. There are others that might be important in particular circumstances.
Also, there may be a positive Babinski sign, which means the great toe in the affected lower extremity moves upward when the bottom lateral surface of the foot is stroked. Normally, the great toe moves downward with this test. Therefore, when an examining doctor says there is a positive Babinski, this is an indication of some type of upper motor neuron lesion. An upper motor neuron lesion may also produce sustained clonus, which is a rhythmic relaxation and contraction of a muscle caused by suddenly stretching a tendon. Clonus is most frequently tested for by a doctor quickly pushing the foot upward to stretch the achilles tendon. Sustained beating movements of the foot are an abnormal clonus indicative of upper motor neuron disease. In addition, muscle tone is increased in upper motor neuron lesions, and, if marked, results in spasticity.
You—or family members or care givers as appropriate—should be asked in detail about your ability to carry out activities of daily living. Of particular interest is your ability to walk up and down steps, the speed at which you walk, and how easily you tire. If you cannot walk a block, you certainly cannot stand and walk 6 to 8 hours daily.
You should also be asked what tasks you could do before your stroke that you cannot do now. Can you dress without assistance? Manipulative functions are important. Can you turn a doorknob? Can you pick up coins and button shirts?